by Dr. M | Mar 12, 2020 | Appointment, Exam, Glaucoma, Mark Moran, Medical Eye Care
As part of your comprehensive eye exam, we check the pressure of your eye, the Intraocular Pressure (IOP). This test, called tonometry, is one way to see if you are at risk for glaucoma. Regular screenings are a simple way to monitor your eye health. Early detection is essential in the treatment of glaucoma, since many times there are no symptoms with increased pressure, unless it is sudden.
UNDERSTANDING EYE PRESSURE:
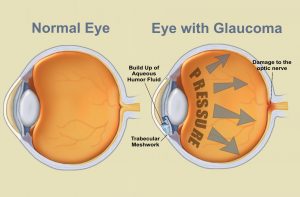
Inside the eye, there is a cycle of fluid production and fluid drainage. This fluid, in the front part of your eye, is called the aqueous humor. The aqueous humor nourishes your eye and helps it to keep its shape. If this cycle is out of balance, and more fluid is produced than can drain effectively, IOP increases. Over time, this increased eye pressure may cause damage to the optic nerve. A general guideline for normal eye pressure is between 10 and 21 mm/hg.
HOW WE MEASURE EYE PRESSURE:
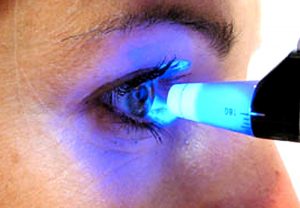 In our office, we measure eye pressure by instilling a drop that numbs your eye. Using a blue light, we then use an applanation tonometer that gently touches the surface of your eye. This painless test is a very effective way of measuring your pressure. It is helpful for the patient to relax and breathe normally while we perform this test.sisipisi.ccsisipisi.ccsisipisi.ccsisipisi.ccsisipisi.cc.
In our office, we measure eye pressure by instilling a drop that numbs your eye. Using a blue light, we then use an applanation tonometer that gently touches the surface of your eye. This painless test is a very effective way of measuring your pressure. It is helpful for the patient to relax and breathe normally while we perform this test.sisipisi.ccsisipisi.ccsisipisi.ccsisipisi.ccsisipisi.cc.
Although there are many other ways of measuring eye pressure, many people are familiar with the “puff of air test”. This test, called non-contact tonometry, uses a rapid air pulse to flatten the cornea. Your pressure is measured by detecting the force of the air against your eye. Although we don’t use this process, often when we ask patients them to “put your chin in the chin rest and forehead against the band” they worry we are going to puff air at them. They don’t seem to like it!
We can’t emphasize enough the importance of comprehensive eye exams. It is especially important to have an eye exam if you have a family history of eye disease, diabetes or high blood pressure. The best way to protect your vision is to come in for an exam, where Dr. Moran will evaluate your risk for disease and advise you of the optimal schedule of visits to protect your eye health.
Schedule your exam today, by calling our office at 610-628-2022, or by filling out the form on the website.
by Dr. M | May 13, 2019 | Appointment, Cost, Diabetes, Exam, Glaucoma, Medical Eye Care, Office, Referral

Health insurance can be very confusing. We talk to patients about it everyday, so we thought it would be helpful to outline the basics.
We can’t stress enough that every plan is different. While you may be covered for a service, you may have a co-pay or deductible that must be paid. If you aren’t sure, please check with your human resources department or insurance company.
MEDICAL INSURANCE: Exams that qualify for Medical Insurance include care and treatment of eye disease and injury. Among the conditions covered are Glaucoma, Cataracts, Diabetic Retinopathy, Macular Degneration, Injury to the Eye, and Infection.
Most medical insurances do NOT cover the cost of checking to see if you need new glasses. This part of the exam is called Refraction (Better 1 or 2?), and is NOT part of medical eye care. Refraction is a separate charge.
VISION INSURANCE: Some benefit plans include vision insurance. Each plan’s coverage is unique, so you need to check specifics with your insurance plan. Items that MAY be covered under vision insurance at a reduced cost or co-pay include your routine eye exam, contact lens fitting, glasses and contact lenses.
Again, we recommend checking with your insurance company to verify your coverage, co-pay and deductible.
We are here to help if you need any treatment information or diagnosis codes so that you can discuss specifics with your insurance provider.
Ultimately, your insurance company considers you responsible to investigate your coverage and will often only provide that information to you, not to your doctor.
by Dr. M | Jan 3, 2019 | Appointment, Diabetes, Dilation, Exam, Glaucoma, Low Vision, Macula, Mark Moran, Medical Eye Care, Patient Care, Retina
Your annual eye exam offers a look at more than just your vision.
You may have heard that the eyes are the windows to your soul, but did you know that they provide a look at your overall health as well.
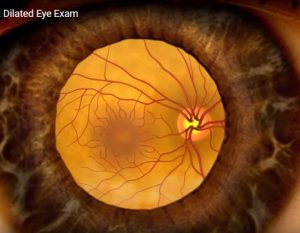
Your dilated eye is an open window where blood vessels and nerves can be clearly seen. The view through the open pupil is a unique means of detecting health issues including:
Your eye doctor may be the first to alert you to developing health problems.The American Optometric Society reported that in just one year, over 250,000 patients were diagnosed with diabetes after their optometrists reported concerns. Early diagnosis and treatment are vital for the health and vision of diabetic patients.
Changes or fluctuation in your vision may also be an indicator of a larger health problem. Report blurred vision to your eye doctor, it may be a sign of increased blood sugar levels and the need for medical treatment.
Uncontrolled diabetes can have severe consequences. Loss of vision due to diabetic retinopathy is a primary concern. Diabetes is the leading cause of blindness in people under the age of 74, so a regular schedule of dilated eye exams are important for diabetic patients. If you know someone who is diabetic,or has a family history of the disease, make sure that they are getting the eye care that they need.
Our goal is to keep you healthy!
Dr. Moran and Dr. Tang not only provide excellent vision care, they are essential partners for your general health and well-being. If you are overdue for a vision exam, don’t delay. Call us to schedule your appointment, Monday through Friday from 8 am to 4 pm.
For a video of a dilated eye exam, click here National Eye Institute Dilated Eye Exam
by Dr. M | Dec 27, 2018 | Cataracts, Contact Lenses, Diabetes, Dry Eye, Eye Safety, Eyeglasses, Floaters, Glasses, Glaucoma, LASIK, Low Vision, Macula, Procedure, Retina, Surgery, Vision
A patient asked the other day, “Do you do regular eye exams?”
Of course we do! At Moran Eye Associates we offer Complete Eye Care, which includes Vision, Medical and Surgical services.

Better 1 or 2?
VISION: We accept VSP & NVA
- Routine Eye Exams
- Contact Lenses: Traditional & Specialty Lenses
MEDICAL: We accept most medical insurancessisipisi.ccsisipisi.ccsisipisi.ccsisipisi.cc
- Diabetic Eye Care: Diabetic Retinopathy
- Glaucoma Care: Medical and Surgical Treatment Options
- Macular Degeneration
- Dry Eye Treatment: Diagnostic Services & Thermal Therapy
- Eye Emergencies
- Infection/Inflammation
- Low Vision Services
SURGICAL: Dr. Moran does surgery at the Surgery Center of Allentown, Sightpath LASIK Center in Bethlehem, as well as some procedures in our Delaware Avenue office.
- Cataracts
- LASIK
- PRK
- Laser Floater Removal
- Glaucoma Eye Surgery
- Foreign Body Removal
- Eye Lid Surgery
Please contact our office if you need an appointment for your eye care. Call or text us at 610-628-2022, or send us an email by filling out the form on the right!
by Dr. M | Oct 23, 2018 | Cataracts, Cost, Education, Exam, Glaucoma, Mark Moran, Medical Eye Care, Procedure, Surgery
The iStent Inject: This procedure may eliminate the need for daily glaucoma drops!

Size of the iStent Inject
Dr. Mark Moran is now offering Micro-Invasive Glaucoma Surgery (MIGS) with the iStent Inject. This option is currently available for glaucoma patients who are having cataract surgery.
Clinical studies have shown a significant decrease in eye pressure in mild-to-moderate glaucoma with this implant. It is interesting to note that the iStent Inject is the smallest medical device known to be implanted in the human body. The picture to the right shows the actual iStent as a tiny speck on the face of a penny!
An Alternative to Glaucoma Drop Therapy
If using drops to control your glaucoma poses problems for you, this procedure may be a great alternative. Ask yourself if you have these issues with your glaucoma medication:
- Do you have problems putting drops in your eyes?
- Do you forget to use your drops as prescribed?
- Do you have financial concerns with the cost of prescription drops?
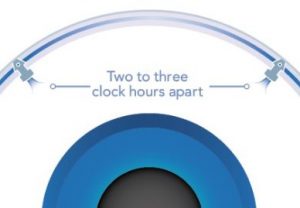
iStent Inject in place
How the iStent works: During cataract surgery, Dr. Moran inserts these tiny stents to create two openings between the front part of the eye and the eye’s natural drainage pathway. This improved flow decreases the pressure in the eye.
Insertion of this FDA approved device is painless. You won’t be able to see or feel these microscopic devices. They are so small that you won’t have to worry about going through an airport metal detector or having an MRI.
This combined cataract/stent procedure does not significantly increase the amount of time that you will spend in the operating room. The recovery time from this procedure is the same as with cataract surgery alone.
Dr. Moran explains the results: “I’ve seen a decrease in pressure in the patients who have had the stents inserted. Many have stopped using their drops altogether. We remind patients that this stent procedure is a treatment, NOT a cure for glaucoma. You still need to follow up with regular appointments to monitor your glaucoma, and maintain the health of your eyes.”
If you have questions about glaucoma, cataracts, or any other vision concern, call to make an appointment at 610-628-2022. Dr. Moran and Dr. Tang would be happy to review your history and discuss if this procedure is right for you.
by Dr. M | Sep 19, 2018 | Dry Eye, Education, Exam, Experience, Glaucoma, Low Vision, Mark Moran, Medical Eye Care, Patient Care, Vision
 The certificate has arrived, so now it is official!
The certificate has arrived, so now it is official!
Bobbi Spain has received her COA designation from the International Joint Commission on Allied Health Personnel in Ophthalmology (JCAPHO). Bobbi is our surgical coordinator, who works with LASIK and cataract patients. She was surprised to see that the package from JCAPHO also included an official COA card, pin and patch!

Official Certification
To provide the best care for our patients, the staff at Moran Eye Associates makes learning a priority. Every member of the team takes part in monthly compliance training, as well as taking on additional programs of study in general ophthalmology, low vision, dry eye management, regulations and billing. They also attend industry conferences each year to keep up with advances in technology and and patient care.
In 2017, Mandy, Beth and Dr. Moran attended the American Academy of Ophthalmology (AAO) conference in New Orleans. In April of this year, Bobbi and Cindy accompanied Dr. Moran to the American Society of Cataract and Refractive Surgeons (ASCRS) in Washington, D.C.

Bobbi joins Mandy and Cindy, who already have their COA certificates on display. Mandy received her COA in 2017. Cindy has been a COA since 2004. In order to maintain certification, a total of 18 credits in continuing education must be completed every three years. Eighteen credits is an easy to complete at Moran Eye Associates, where continuing education plays a key role in our success!


 In our office, we measure eye pressure by instilling a drop that numbs your eye. Using a blue light, we then use an applanation tonometer that gently touches the surface of your eye. This painless test is a very effective way of measuring your pressure. It is helpful for the patient to relax and breathe normally while we perform this test.
In our office, we measure eye pressure by instilling a drop that numbs your eye. Using a blue light, we then use an applanation tonometer that gently touches the surface of your eye. This painless test is a very effective way of measuring your pressure. It is helpful for the patient to relax and breathe normally while we perform this test.



 The certificate has arrived, so now it is official!
The certificate has arrived, so now it is official!
